Autotransfusion
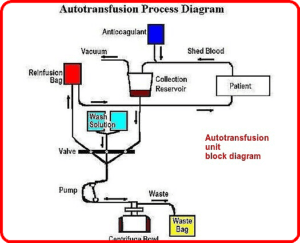
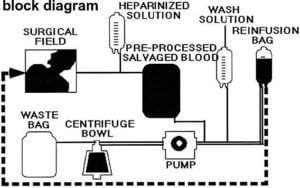
Autotransfusion units are designed to collect and process blood lost by a patient to extract red blood cells (RBCs) for subsequent transfusion into the same patient. They are particularly intended for use in surgeries that involve a substantial volume of blood loss. Autotransfusion is a process wherein a person receives their blood for a transfusion, instead of banked allogenic (separate-donor) blood.
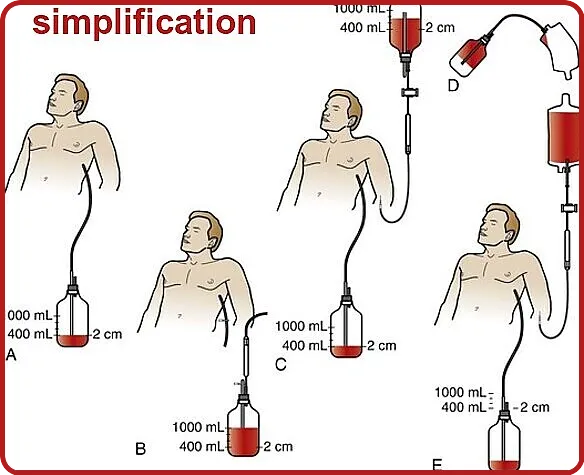
Autotransfusion is most commonly used in the emergency department in trauma patients with evidence of a significant hemothorax. If the patient’s signs and symptoms display evidence of hemothorax preparation of autotransfusion should begin urgently before chest tube placement.

Basic components
a. Collection reservoir
b. Roller pump
c. Centrifuge bowl
d. Air detector
e. Microfilter
Basic principles
1. Use of autotransfusion devices requires aspiration of extravascular blood from the surgical site into the collection reservoir of the unit, where it undergoes gross filtration.
2. To keep the blood from clotting while in the unit, an anticoagulant (heparin) is added to the aspiration line at a rate proportional to the rate of blood collection.
3. From the reservoir, the unit’s roller pump sends the blood into a centrifuge
bowl.
4. Once the bowl is full, the pump shuts off and the RBCs are spun and washed with normal saline to remove anticoagulant.
5. The saline wash is monitored by an air detector.
6. When a saline bag is depleted during the wash cycle, residual air in the saline bag is detected by the air detector, triggering an alarm to alert the operator to replace the bag.
7. During the wash cycle, the saline flows into a waste bag, leaving the packed RBCs in the centrifuge bowl.
8. RBCs are then pumped into a holding bag for reinfusion and delivered to the patient through a microfilter.
9. Operate in an automatic or a manual mode.
10. Automatic mode is most often used for routine procedures; the operator simply selects a programmed cycle choice with preset wash volumes and pumping rates and initiates the cycle.
11. The system detects when the bowl is full, automatically triggering the separation and wash cycle.
12. High-speed processing units can process one unit of packed red cells (250 ±50 mL) in about three minutes; faster cycle times typically yield less efficient washes.
13. A manual mode allows operators to control the start of each processing stage and the saline volume in wash cycles for maximum flexibility in exceptional cases.
14. Faster cycle times can be achieved in this mode because wash cycles can be eliminated if rapid reinfusion is necessary; however, the operator should try increasing pump speeds before choosing to eliminate wash cycles to avoid giving patients potentially contaminated blood.