What is the Pulmonary analyzers?
The word “pulmonary analyzers” is a general one that may be used to describe a wide range of apparatus or medical devices that are used to evaluate and analyze lung function. These tools are essential for identifying respiratory disorders, keeping an eye on lung health, and assessing how well respiratory treatments are working. Some popular varieties of pulmonary analyzers are as follows:
- Spirometer:
- A spirometer is a device used to measure lung function by assessing the volume and flow of air during inhalation and exhalation. It is commonly used to diagnose and monitor respiratory conditions such as asthma, chronic obstructive pulmonary disease (COPD), and interstitial lung diseases.
- Peak Flow Meter:
- A peak flow meter is a handheld device that measures the maximum airflow a person can generate during a forceful exhalation. It is often used by individuals with asthma to monitor changes in airflow and assess the effectiveness of asthma management.
- Gas Analyzers:
- Gas analyzers are devices that measure the concentration of gases in the respiratory system, particularly oxygen and carbon dioxide. These analyzers are used in settings such as pulmonary function testing and arterial blood gas analysis to assess respiratory and metabolic status.
- Pulse Oximeter:
- While not exclusively a pulmonary analyzer, a pulse oximeter is commonly used to measure the oxygen saturation levels in the blood. It is a non-invasive device that clips onto a person’s fingertip, providing information about how well the lungs are oxygenating the blood.
- Exhaled Nitric Oxide (FeNO) Analyzer:
- This analyzer measures the concentration of nitric oxide in a person’s exhaled breath. Elevated levels of exhaled nitric oxide may be associated with airway inflammation, making this test useful in the diagnosis and management of asthma.
- Body Plethysmography:
- This advanced pulmonary function test involves a person sitting inside a sealed chamber to measure lung volumes and airway resistance. It provides comprehensive information about lung function and is often used in the evaluation of respiratory conditions.
- Impulse Oscillometry:
- This technique assesses lung function by measuring the resistance and reactance of the respiratory system in response to pressure oscillations. It is useful in detecting changes in airway function, especially in patients who may have difficulty performing traditional spirometry.
- Capnograph:
- A capnograph measures the concentration of carbon dioxide in exhaled breath. It is commonly used in medical settings, including during anesthesia and in the management of patients with respiratory conditions.
Article About:- Health & fitness
Article About:- Medical Technolo
Article About:- Sports

How to Work with a Pulmonary Analyzer
Working with a pulmonary analyzer involves using specific devices to assess and measure various aspects of pulmonary (lung) function. Below are general steps that individuals or healthcare professionals may follow when working with common pulmonary analyzers:
Spirometer:
- Preparation:
- Ensure that the spirometer is clean and calibrated according to the manufacturer’s instructions.
- Instruct the individual to sit comfortably with proper posture.
- Patient Instructions:
- Explain the procedure to the individual and provide clear instructions for inhalation and exhalation maneuvers.
- Instruct the individual to take a maximal inhalation followed by a forceful exhalation into the spirometer.
- Spirometry Test:
- Start the spirometry test, and observe the individual’s effort during inhalation and exhalation.
- The spirometer records parameters such as forced vital capacity (FVC), forced expiratory volume in one second (FEV1), and other lung volumes.
- Repeat Testing:
- Conduct multiple trials to ensure consistency and obtain reliable results.
- Evaluate the spirometry curves and values to assess lung function.
- Interpretation:
- Interpret the spirometry results in conjunction with reference values and clinical context.
- Identify any abnormalities or patterns indicative of respiratory conditions.
Peak Flow Meter:
- Baseline Measurement:
- Establish a baseline peak flow measurement for the individual.
- Ensure the peak flow meter is set to zero.
- Patient Instructions:
- Instruct the individual to stand or sit upright and take a deep breath.
- Place the mouthpiece securely in the mouth, forming a tight seal.
- Forceful Exhalation:
- Instruct the individual to exhale forcefully into the peak flow meter.
- Record the peak flow measurement.
- Repeat Monitoring:
- Repeat the process multiple times to monitor variability.
- Record the highest peak flow value obtained.
- Interpretation:
- Compare the recorded peak flow values with the individual’s personal best or predicted values.
- Assess for changes that may indicate worsening lung function or the need for adjustments in asthma management.
Pulse Oximeter:
- Preparation:
- Ensure the pulse oximeter is clean, functional, and has fresh batteries if needed.
- Warm the individual’s hands if they are cold to enhance blood flow.
- Sensor Placement:
- Place the pulse oximeter sensor on a fingertip, earlobe, or other suitable site.
- Ensure a secure fit without excessive pressure.
- Patient Instructions:
- Instruct the individual to remain still and avoid moving the hand with the sensor during the measurement.
- Recording:
- The pulse oximeter will display the oxygen saturation (SpO2) and pulse rate.
- Record the values after a stable reading is obtained.
- Interpretation:
- Interpret the SpO2 and pulse rate in the context of the individual’s baseline and clinical condition.
- Assess for any signs of oxygen desaturation.
Specific Pulmonary Function Tests
- Preparation:
- Follow specific guidelines for the preparation and calibration of the chosen pulmonary function test.
- Patient Instructions:
- Provide clear instructions to the individual about the specific maneuvers required for the test.
- Conducting the Test:
- Perform the test according to the established protocol, monitoring the individual’s effort and cooperation.
- Data Collection:
- Record the relevant parameters measured by the specific pulmonary function test.
- Interpretation:
- Interpret the results in consultation with reference values and clinical guidelines.
- Use the information obtained to assess lung function and guide further management.
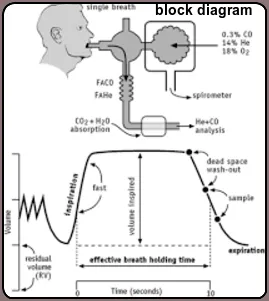
This test is done by having you take in a deep breath and then, as fast as you can, blow out all of the air. You will be blowing into a tube connected to a machine (spirometer). To get the “best” test result, the test is repeated three times. You will be given a rest between tests. Pulmonary function analyzers measure the performance of a patient’s respiratory system, especially for outpatient or presurgical screening.
These systems measure the ventilation, diffusion, and distribution of gases in the lungs. They are used to help assess patients with conditions like chronic obstructive pulmonary disorder (COPD).
What is the working principle of pulmonary analyzers?
Spirometry instruments measure the volume of gases exhaled by the patient (volume changes of the lungs) either by volume displacement or flow sensing methods. Spirometers measure the volume directly; these devices include water-seal bellows and rolling-seal spirometers, or the flow of gas that is integrated to yield volume. Such flow sensing instruments can employ a pneumotachometer, a hot-wire anemometer, or a turbine meter. Some analyzers incorporate computers with software that permits customized reports or the inclusion of specialized predictive equations for normal function.

What are the methods used to measure pulmonary function?
Pulmonary analyzers encompass various devices designed to assess and measure different aspects of lung function. Each type of pulmonary analyzer operates based on specific principles relevant to its intended function. Here are the working principles of some common pulmonary analyzers:
Spirometer:
- Principle:
- A spirometer measures lung volumes and airflow by analyzing the volume of air breathed in and out during specific respiratory maneuvers.
- Operation:
- The individual inhales and exhales into the spirometer, causing changes in the volume of air within the device.
- The spirometer records the changes in volume over time, generating a spirometry curve.
- Parameters such as Forced Vital Capacity (FVC), Forced Expiratory Volume in one second (FEV1), and others are calculated based on the spirometry curve.
Peak Flow Meter:
- Principle:
- A peak flow meter measures the maximum speed of air expelled from the lungs during a forceful exhalation.
- Operation:
- The individual exhales forcefully into the peak flow meter.
- The peak flow meter measures the highest flow rate achieved during the exhalation.
- The recorded value represents the peak expiratory flow (PEF).
Pulse Oximeter:
- Principle:
- A pulse oximeter measures the oxygen saturation (SpO2) of arterial blood by analyzing the absorption of light by oxygenated and deoxygenated hemoglobin.
- Operation:
- The pulse oximeter emits two wavelengths of light (usually red and infrared) through a pulsatile vascular bed (e.g., fingertip).
- Oxygenated hemoglobin absorbs light differently than deoxygenated hemoglobin, allowing the device to calculate the ratio and determine oxygen saturation.
- The pulse rate is derived from the pulsatile component of the arterial blood.
Exhaled Nitric Oxide (FeNO) Analyzer:
- Principle:
- This analyzer measures the concentration of nitric oxide in exhaled breath, which is associated with airway inflammation.
- Operation:
- The individual exhales into the FeNO analyzer.
- The device detects and quantifies the concentration of nitric oxide in the exhaled breath, providing information about airway inflammation.
Body Plethysmography:
- Principle:
- Body plethysmography measures lung volumes and airway resistance by analyzing changes in pressure and volume within an enclosed chamber.
- Operation:
- The individual sits inside the plethysmography chamber.
- During respiratory maneuvers (e.g., breathing in and out against a closed shutter), changes in pressure and volume within the chamber are measured.
- These measurements allow for the calculation of lung volumes and airway resistance.
Impulse Oscillometry:
- Principle:
- Impulse oscillometry measures respiratory system resistance and reactance by applying pressure oscillations during tidal breathing.
- Operation:
- The individual breathes normally while pressure oscillations are introduced.
- The device analyzes the resistance and reactance of the respiratory system based on the response to the pressure oscillations.

What are the different types of pulmonary function tests?
Pulmonary function tests (PFTs) are a group of diagnostic tests that assess the function of the respiratory system, including the lungs and airways. These tests provide valuable information about lung volumes, capacities, rates of flow, and gas exchange. Here are different types of pulmonary function tests:
Spirometry:
- Purpose: Measures the amount of air an individual can inhale or exhale and the rate of airflow.
- Parameters: Forced Vital Capacity (FVC), Forced Expiratory Volume in one second (FEV1), FEV1/FVC ratio, Peak Expiratory Flow (PEF).
Peak Flow Measurement:
- Purpose: Measures the maximum speed of air expelled during a forceful exhalation.
- Parameters: Peak Expiratory Flow (PEF).
Lung Volumes and Capacities:
- Purpose: Assesses the amount of air in the lungs and how well the lungs expand and contract.
- Parameters: Total Lung Capacity (TLC), Residual Volume (RV), Functional Residual Capacity (FRC), Inspiratory Capacity (IC).
Diffusion Capacity Testing (DLCO):
- Purpose: Measures the ability of the lungs to transfer gases, particularly oxygen, from the air into the bloodstream.
- Parameters: Diffusing Capacity of the Lung for Carbon Monoxide (DLCO).
Body Plethysmography:
- Purpose: Measures lung volumes, airway resistance, and other respiratory parameters using an enclosed chamber.
- Parameters: Total Lung Capacity (TLC), Residual Volume (RV), Specific Airway Conductance (sGaw).
Impulse Oscillometry:
- Purpose: Measures respiratory system resistance and reactance during tidal breathing.
- Parameters: Resistance at various frequencies, Reactance at various frequencies.
Arterial Blood Gas (ABG) Analysis:
- Purpose: Evaluates the oxygen and carbon dioxide levels in arterial blood.
- Parameters: Partial Pressure of Oxygen (PaO2), Partial Pressure of Carbon Dioxide (PaCO2), pH, Bicarbonate (HCO3-).
Exhaled Nitric Oxide (FeNO) Measurement:
- Purpose: Measures the concentration of nitric oxide in exhaled breath, indicating airway inflammation.
- Parameters: Fractional Exhaled Nitric Oxide (FeNO).
Six-Minute Walk Test:
- Purpose: Assesses exercise tolerance and oxygen saturation during a six-minute walk.
- Parameters: Distance walked, Oxygen saturation.
Methacholine Challenge Test:
- Purpose: Evaluates airway hyperresponsiveness in individuals with suspected asthma.
- Parameters: Changes in lung function following inhalation of methacholine.
Exercise Stress Test:
- Purpose: Assesses respiratory responses during exercise.
- Parameters: Changes in lung function, oxygen saturation during exercise.
Bronchial Provocation Test:
- Purpose: Measures changes in lung function in response to inhaled substances (e.g., allergens) to identify respiratory sensitivity.
- Parameters: Changes in FEV1.
Pulse Oximetry:
- Purpose: Measures oxygen saturation in peripheral blood.
- Parameters: Oxygen saturation (SpO2), Pulse rate.
What are the most commonly used PFT tools?
The following is a list of the most common types of PFT devices used in a clinical setting:
Pressure plethysmograph.
Flow plethysmograph.
Pulmonary gas analyzer.
Oxygen Analyzer.
Gas conditioning device.
Blood gas analyzer.
Silverman Pneumotachometer.
ultrasonic spirometer
What is the difference between Pulmonary Function Test and Spirometry?
The difference between these two is as follows: Pulmonary function testing shows how well you are breathing. This allows a variety of pulmonary function tests to be performed. Spirometry is a type of pulmonary function test. Spirometry is a simple test to measure how much (volume) and how fast (flow) air you can move in and out of your lungs.

How do you test your lung capacity at home?
One common method is to use a peak flow meter, a handheld device that measures the strength of your breath. You simply breathe in from one end and the meter immediately shows a reading on a scale, usually in liters per minute (LPM).
What is poor pulmonary function?
The term “poor lung function” includes various chronic diseases with different mechanisms of atherothrombosis. Research is needed to better understand why individuals with lung dysfunction are at higher cardiovascular risk, and to identify adequate preventive strategies.
What are pulmonary risk factors?
Risk Your risk of getting PAH is higher if two or more family members have PAH or if a family member in your lineage has a gene linked to PAH. ,
1. Obesity and obstructive sleep apnea.
2. gender.
3. pregnancy.
4. Height.
5. other diseases.
6. Drugs and toxins.
Highest risk factor Smoking is the biggest risk factor for chronic obstructive pulmonary disease (COPD), which includes chronic bronchitis and emphysema.
What is the benefit of pulmonary function?
Pulmonary function tests (PFTs) provide valuable information about the function of the respiratory system, including the lungs and airways. The benefits of pulmonary function testing are numerous and play a crucial role in the diagnosis, management, and monitoring of respiratory conditions. Here are some key benefits:
- Diagnosis of Respiratory Conditions:
- PFTs help diagnose various respiratory disorders, including asthma, chronic obstructive pulmonary disease (COPD), interstitial lung diseases, bronchiectasis, and restrictive lung diseases.
- Assessment of Lung Function:
- PFTs quantify lung volumes, capacities, and rates of airflow, providing a comprehensive assessment of how well the lungs expand and contract. This information helps identify abnormalities in lung function.
- Evaluation of Disease Severity:
- PFT results help determine the severity of respiratory conditions, guiding healthcare professionals in developing appropriate treatment plans and interventions.
- Monitoring Disease Progression:
- Repeat PFTs over time help monitor changes in lung function, allowing healthcare providers to assess disease progression and adjust treatment strategies accordingly.
- Treatment Planning and Optimization:
- PFT results guide healthcare professionals in tailoring treatment plans to address specific patterns of lung dysfunction. Medications, pulmonary rehabilitation, and other therapeutic interventions can be optimized based on PFT findings.
- Assessment of Response to Treatment:
- PFTs are used to assess how well a patient responds to prescribed treatments, such as bronchodilators or anti-inflammatory medications. Improvement in lung function indicates a positive response to therapy.
- Identification of Lung Abnormalities:
- PFTs can identify specific patterns of lung abnormalities, such as airflow obstruction, restrictive lung disease, or impaired gas exchange, aiding in the identification of the underlying cause.
- Preoperative Assessment:
- Prior to surgery, especially for procedures involving the chest or respiratory system, PFTs help assess the patient’s baseline lung function and identify potential risks during and after surgery.
- Workplace and Environmental Exposure Evaluation:
- PFTs are used in occupational medicine to assess the impact of workplace or environmental exposures on lung function, helping to identify potential hazards and guide preventive measures.
- Screening for Lung Disease in High-Risk Populations:
- PFTs may be used for screening purposes in high-risk populations, such as smokers or individuals with a family history of lung disease, to detect early signs of respiratory abnormalities.
- Exercise Capacity Assessment:
- Some PFTs, like the six-minute walk test, assess exercise tolerance and oxygen saturation during physical activity, providing insights into overall respiratory health.
- Patient Education and Management Planning:
- PFTs contribute to patient education by helping individuals understand their lung function and the impact of respiratory conditions on their health. This understanding is crucial for effective self-management.
FAQ
How is pulmonary function measured?
A range of tests are used to assess the functionality of the lungs, collectively referred to as pulmonary function tests or lung function assessments. A spirometry test is the most basic. This test determines how much air the lungs can contain. The exam also assesses the degree of power required to expel air from the lungs.
What are the 3 parts of a pulmonary function test?
Spirometry, lung volume measurement, and lung diffusion capacity are the three primary PFT kinds.
Spirometry. The rate of airflow into and out of the lungs is measured by spirometry.
testing of the lung volume.
lung’s ability to diffuse.
oximetry of the pulse.
checking for arterial blood gas.
What is breath analyzer lung function?
Your lips will be firmly sealed around a mouthpiece that is attached to a spirometer. It will be instructed for you to inhale deeply and exhale as forcefully as possible into the mouthpiece. The amount and rate at which you exhale will be recorded by the spirometer.
What is the full form of PFT?
The pulmonary function test (PFT) assesses the lung function. The test gauges the child’s capacity to hold air in his or her lungs as well as the efficiency with which they can expel it.
What is the pulmonary test for COPD?
To diagnose COPD, a spirometry test is used. You can gauge how much and how quickly you exhale air with a spirometer. This makes it easier for your doctor to assess how well your lungs are functioning. Individuals with COPD diagnosis, irrespective of age or race, have to undergo testing for AAT deficiency.




Comments
One response to “What is the Pulmonary analyzers: Working Principle, Uses and Best Benefit Risk24”